Neonatal Jaundice Why occurs ?
Neonatal Jaundice Cause, Pathogenesis Diagnosis and Treatment
Introduction
Neonatal jaundice is a common condition in newborns characterized by the yellowing of the skin and eyes. Understanding the causes, symptoms, and management of neonatal jaundice is crucial for the well-being of newborns.
In this article, we will explore the various aspects of neonatal jaundice and provide insights into what it is, why it occurs, how it can be managed, and when to seek medical attention. “According to leading pediatricians, neonatal jaundice affects up to 60% of newborns worldwide.
Definition of Neonatal Jaundice
Neonatal jaundice refers to the yellow discoloration of a newborn’s skin and eyes caused by elevated levels of bilirubin in the blood. Bilirubin is a yellow pigment produced when red blood cells break down. In healthy individuals,
the liver processes and eliminates bilirubin from the body. However, in newborns, the liver is not fully developed, resulting in the accumulation of bilirubin and the subsequent appearance of jaundice.
Causes of Neonatal Jaundice
A. Physiological Jaundice
Physiological jaundice is the most common type of jaundice in newborns and typically appears 2-3 days after birth. It is caused by the increased breakdown of red blood cells and the immaturity of the liver, which hinders the processing of bilirubin.
B. Pathological jaundice
Pathological jaundice is a type of jaundice that occurs in newborns and is caused by underlying medical conditions. pathological jaundice is characterized by higher levels of bilirubin and may require medical intervention. Pathological jaundice often appears within the first 24 hours of birth or persists beyond two weeks.
Factor of Cause Neonatal Jaundice
Breast Milk Jaundice
In some cases, breastfeeding can contribute to jaundice. Certain substances in breast milk can interfere with the liver’s ability to process bilirubin effectively, leading to its accumulation in the baby’s body.
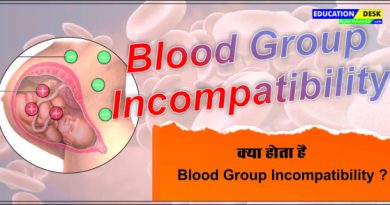
If the mother and baby have different blood types, it can result in a condition called hemolytic disease of the newborn. This occurs when the mother’s antibodies attack the baby’s red blood cells, leading to an increased breakdown of these cells and subsequent jaundice.
Premature Birth:
Premature infants are more susceptible to jaundice because their livers may not be fully matured.
Highest Number of RBCs
Highly Break Down RBCs as maintain a Normal value of RBCs and in Birth child RBC life Span 60-70 day
Pathogenesis of Neonatal Jaundice
Increased Bilirubin Production: Neonatal jaundice typically occurs due to an increased breakdown of red blood cells. This process leads to an elevated production of bilirubin, the pigment responsible for the yellow discoloration. The immature liver of a newborn may struggle to process and eliminate bilirubin efficiently, contributing to its accumulation.
Immature Liver Function: The liver plays a vital role in the metabolism and elimination of bilirubin. In newborns, the liver is not fully developed and may have reduced enzymatic activity. As a result, bilirubin conjugation, the process of converting unconjugated bilirubin into a water-soluble form for excretion, may be impaired.
Also Read this Article
What is relation between Hypertension and Kidney ?
Confirming Anemia: Diagnostic Tests and Symptoms
Symptoms and Signs
A. Yellowing of the skin and eyes
The primary symptom of neonatal jaundice is the yellow discoloration of the skin and eyes. This yellowing, also known as icterus, typically starts from the face and then progresses downward to the chest, abdomen, and extremities.
B. Other associated symptoms
In addition to yellowing, other symptoms may include poor feeding, lethargy, dark urine, pale stools, and a high-pitched cry.
C. When to seek medical attention
It is important to seek medical attention if the jaundice appears within the first 24 hours after birth, if the baby’s skin develops a deep yellow or orange color, if the baby becomes lethargic or irritable, or if the jaundice persists beyond two weeks.

Management of Neonatal Jaundice
A. Phototherapy
Phototherapy is a widely used treatment for neonatal jaundice. It involves exposing the baby’s skin to a specific type of light that helps break down bilirubin into a more easily excretable form. This treatment is non-invasive and generally safe.
B. Exchange Transfusion
In severe cases of jaundice, where the bilirubin levels are dangerously high, an exchange transfusion may be necessary. This procedure involves replacing the baby’s blood with compatible donor blood to reduce the bilirubin levels.
C. Increased Feeding
In cases of breastfeeding-related jaundice, increasing the frequency of feeding can help eliminate bilirubin from the baby’s system more effectively. The colostrum in breast milk acts as a natural laxative, aiding in the elimination of bilirubin through the stools.
Prevention and Early Detection
To prevent neonatal jaundice, regular check-ups during pregnancy are essential. These check-ups allow healthcare professionals to monitor the baby’s development and identify any risk factors that may contribute to jaundice. Monitoring bilirubin levels after birth and early intervention when necessary can also help prevent complications.
FAQs (Frequently Asked Questions)
A. Can neonatal jaundice be prevented?
While neonatal jaundice cannot always be prevented, ensuring regular check-ups during pregnancy and after birth can help monitor the baby’s bilirubin levels and detect any potential issues early on.
B. Is neonatal jaundice a serious condition?
In most cases, neonatal jaundice is not a serious condition and resolves on its own. However, severe jaundice can lead to complications, such as brain damage, if left untreated.
C. How long does neonatal jaundice last?
Physiological jaundice typically resolves within two weeks. However, in some cases, jaundice may persist for a longer duration, requiring further evaluation and management.
D. Can breastfeeding cause neonatal jaundice?
Breastfeeding can contribute to neonatal jaundice in some cases. However, it is important to note that breastfeeding-related jaundice is generally mild and resolves with increased feeding.
E. Is neonatal jaundice contagious?
No, neonatal jaundice is not contagious. It is a physiological condition that occurs due to the normal breakdown of red blood cells in newborns.
F. Are there any long-term effects of neonatal jaundice?
In most cases, neonatal jaundice does not cause any long-term effects. However, severe or untreated jaundice can lead to complications, such as kernicterus, which can result in brain damage.
Conclusion
Neonatal jaundice is a common condition in newborns, characterized by yellowing of the skin and eyes due to elevated levels of bilirubin. While generally harmless, it is essential to understand the causes, symptoms,
and management of neonatal jaundice to ensure the well-being of the baby. Regular check-ups, early detection, and appropriate interventions are key to preventing complications and promoting a healthy start to life.
This is only for Educational Purpose


Pingback: Hair fall and blood test for hair loss » Digital Hybrid Education
Pingback: Mechanism of Bilirubin production and type of Bilirubin » Digital Hybrid Education